Vaccinating against Hepatitis B
The epidemiological curves comparing pre- and post-vaccination periods show a sharp decrease in the number of cases over the years. It is clear that vaccinations have significantly changed the incidence of diseases for which immunisation exists, thus saving lives, reducing disease outcomes, reducing overall population suffering and improving quality of life.
The disease before and after the vaccination campaign in Italy
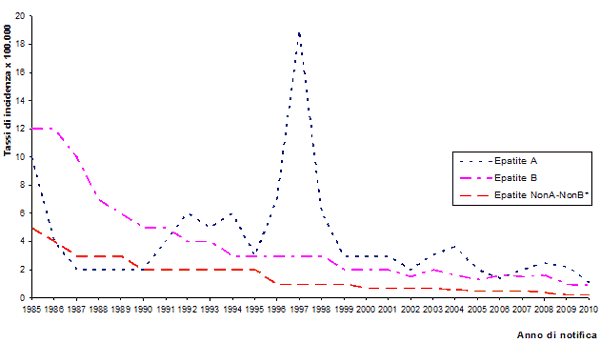
Figure 1 shows the incidence rates per 100,000 of hepatitis A, B and C, per year. Data Seieva 1985-2010
* Since 2009, Hepatitis C
Over time, infections of HBV virus (always transmitted via blood, as with hepatitis C and Delta) have shown a significant reduction in incidence, reaching in 2010 values of 0.9 per 100,000 (respectively 0.0, 0.5 , and 1,2, for the age groups 0-14, 15-24, and ≥ 25). For the HBV virus, (as for the HCV virus, this can be attributed to various causes: improved hygienic and socio-economic conditions, smaller family sizes and therefore a reduced intra-family spread of the viruses, a greater knowledge regarding transmission routes and better prevention with the introduction of measures such as blood screening, screening for HBsAg in pregnant women and prophylaxis for babies born to HBsAg positive mothers, the adoption of universal precautions (in particular the use of disposable syringes), and the educational campaign on HIV infection which is spread in the same way as HBV and HCV viruses.
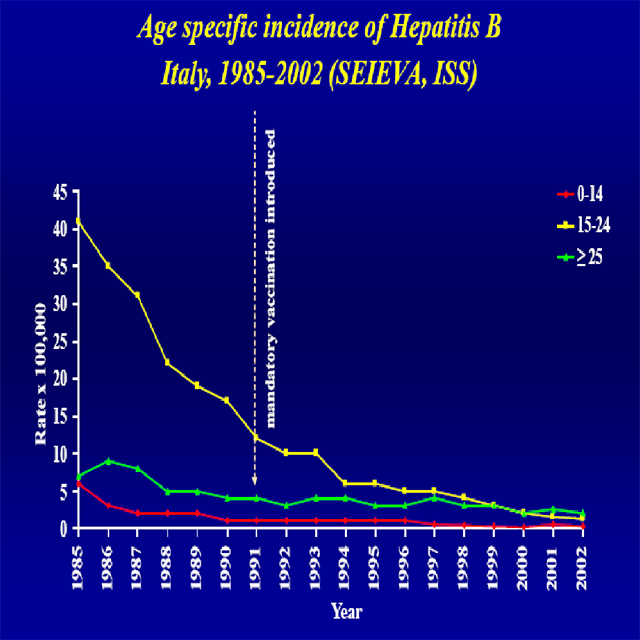
As regards hepatitis B, with the introduction of vaccination, in 1983 for those deemed at high risk of HBV virus infection and made mandatory in 1991 for all newborns and twelve-year-olds, there was a further decline of prevalence and incidence. This decrease in incidence has particularly affected the 15-24 age group, (most likely due to vaccination in 12-year-olds).
Today, hepatitis B occurs more frequently in males. The age-group most affected is 35-54 year-olds. The strongest associations with acute HBV virus infections are now found following percutaneous exposure during cosmetic treatments, dental therapy and promiscuous sexual activity. It should be noted that 17% of acute HBV infections affect immigrants, in particular those from Eastern Europe, an area that is highly endemic for HBV.



